PART 3: Causes and Risk Factors
Why do ear infections and hearing loss happen in the first place?
Many patients assume it is “bad luck.” Others blame ageing alone. The truth is more complex. Ear conditions develop from a mix of anatomy, environment, lifestyle, and health status.
Let’s unpack this clearly.
What Causes Ear Infections?
1. Eustachian Tube Dysfunction
The Eustachian tube connects the middle ear to the back of the nose. It equalises pressure and drains fluid. When it fails, fluid accumulates behind the eardrum.
Blocked drainage creates a perfect breeding ground for bacteria and viruses.
Children are especially vulnerable. Their Eustachian tubes are shorter and more horizontal. That is why ear infections are common in preschoolers.
In Kuala Lumpur, recurrent upper respiratory infections often trigger this dysfunction.

2. Viral and Bacterial Infections
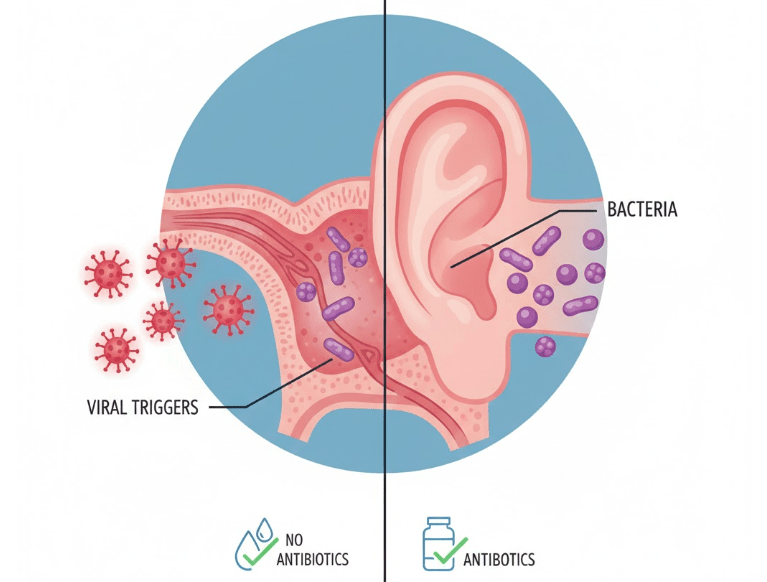
Most middle ear infections begin with a viral cold. The virus causes inflammation. Swelling traps fluid. Bacteria then multiply in that trapped fluid.
Common bacterial organisms have been widely studied in otology journals. However, viral triggers are equally important.
This is why not all ear infections require antibiotics. Evidence-based ENT care now emphasises proper diagnosis before prescribing medication.
3. Humidity and Moisture Exposure
Kuala Lumpur’s tropical climate plays a role.
Persistent humidity encourages fungal and bacterial growth in the ear canal. Swimming, frequent gym sessions, and habitual ear cleaning increase the risk of outer ear infections.
Using cotton buds pushes debris deeper. It also injures the delicate skin of the ear canal. Micro-injuries invite infection.

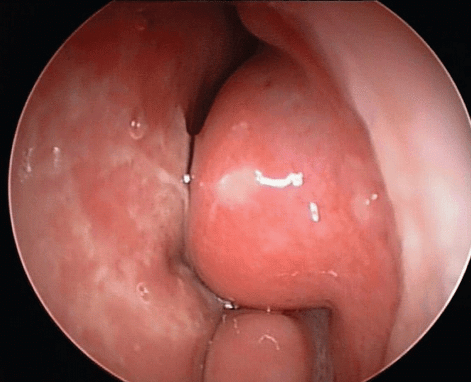
4. Allergic Rhinitis and Sinus Disease
Chronic nasal allergy is extremely common in Malaysia.
Nasal inflammation blocks the Eustachian tube opening. This leads to negative pressure and fluid buildup in the middle ear.
Patients often treat nasal symptoms but ignore subtle ear blockage. Over time, repeated inflammation increases infection risk.
What Causes Hearing Loss?
Hearing loss has broader causes.
1. Age-Related Degeneration (Presbycusis)
Ageing affects the inner ear hair cells. These cells do not regenerate.
After age 50, gradual high-frequency hearing loss becomes common. Urban noise exposure accelerates this process.
In Kuala Lumpur’s busy traffic and construction zones, long-term noise exposure is a significant factor.

2. Noise-Induced Hearing Loss
Loud concerts, headphones at high volume, factory noise, and even motorcycles contribute.
Noise damages the sensory cells inside the cochlea. The damage is often permanent.
Patients rarely notice early signs. They adapt unconsciously.

3. Chronic Ear Infections
Repeated untreated infections may damage the eardrum or ossicles. In severe cases, they erode bone.
Chronic inflammation can also affect the inner ear. This results in mixed or sensorineural hearing loss.
Early intervention prevents this cascade.

4. Medical Conditions
Diabetes, autoimmune disorders, and certain viral infections increase hearing loss risk.
Sudden sensorineural hearing loss, although uncommon, requires emergency ENT evaluation. Delay reduces recovery chances.

5. Ototoxic Medications
Certain medications may affect hearing. These include specific antibiotics and chemotherapy drugs.
Patients often do not associate hearing changes with medication use. Proper monitoring is essential.

Risk Factors Specific to Kuala Lumpur
Urban living introduces unique ENT risks:
- High air pollution levels
- Frequent viral exposure in crowded public transport
- Air-conditioned indoor environments causing nasal dryness
- Recreational noise exposure
- Delayed healthcare visits due to busy schedules
Lifestyle matters.
Ignoring persistent nasal allergy or repeatedly self-medicating for ear pain increases complications.

Why Understanding Causes Changes Outcomes
Knowing the cause changes the strategy.
If allergy drives the problem, treat the nose.
If noise is the culprit, protect the ears.
If infection recurs, evaluate structurally.
Modern ENT practice in Kuala Lumpur focuses on identifying root causes rather than repeatedly prescribing antibiotics.
Because here is the reality:
Untreated risk factors accumulate. Over time, they lead to permanent hearing impairment.
Prevention begins with awareness.
Reviewed by Dr Ameen, ENT Specialist, Kuala Lumpur

References
This article is written based on current evidence and clinical practice standards from leading ENT journals, including The Laryngoscope, JAMA Otolaryngology–Head & Neck Surgery, Otolaryngology–Head and Neck Surgery, Otology & Neurotology, Head & Neck, Clinical Otolaryngology, and European Archives of Oto-Rhino-Laryngology.






























Leave a comment