Diagnosis and Investigations
Let’s be honest.
Many patients assume diagnosing an ear infection is simple. “Doctor, just give antibiotics.” Others believe hearing loss only needs a hearing aid.
But modern ENT diagnosis is far more precise.
In Kuala Lumpur, I frequently see patients treated repeatedly without proper ear examination. The result? Chronic problems that could have been prevented.
Accurate diagnosis is the foundation of effective treatment.

Step 1: Detailed Clinical History
Diagnosis begins before any instrument touches your ear.
I ask about:
– Onset of symptoms
– Duration
– Pain severity
– Hearing changes
– Dizziness
– Previous infections
– Noise exposure
– Medical history
Why does this matter?
Because ear pain with fever differs from ear blockage without pain. Sudden hearing loss differs from gradual decline. The story guides the direction.
Evidence from major otolaryngology journals consistently emphasises structured clinical assessment before intervention.

Step 2: Otoscopic Examination
Next comes direct ear examination.
Using a high-quality otoscope or video otoscope, I inspect:
-Ear canal skin
-Presence of discharge
-Swelling
-Eardrum colour
-Fluid behind the eardrum
-Perforation
A normal eardrum is translucent and slightly pearly. A bulging red eardrum suggests infection. A retracted drum suggests pressure imbalance.
In Kuala Lumpur’s humid climate, fungal infections are not uncommon. These appear distinct from bacterial infections.
Visual clarity changes everything. Guesswork disappears.

Step 3: Hearing Tests (Audiometry)
If hearing loss is suspected, formal hearing tests are essential.
Pure Tone Audiometry
This test measures how well you hear different frequencies. It determines whether hearing loss is conductive, sensorineural, or mixed.
This distinction is critical.
Fluid behind the eardrum causes conductive loss. Inner ear damage causes sensorineural loss. Treatment differs completely.
Speech Audiometry
This measures clarity of speech recognition. Many patients say, “I hear but don’t understand.” This test explains why.
Tympanometry
This assesses eardrum mobility. It detects middle ear fluid or pressure problems. It is particularly useful in children with suspected silent fluid.
Modern ENT practice in Kuala Lumpur relies heavily on these objective tools.
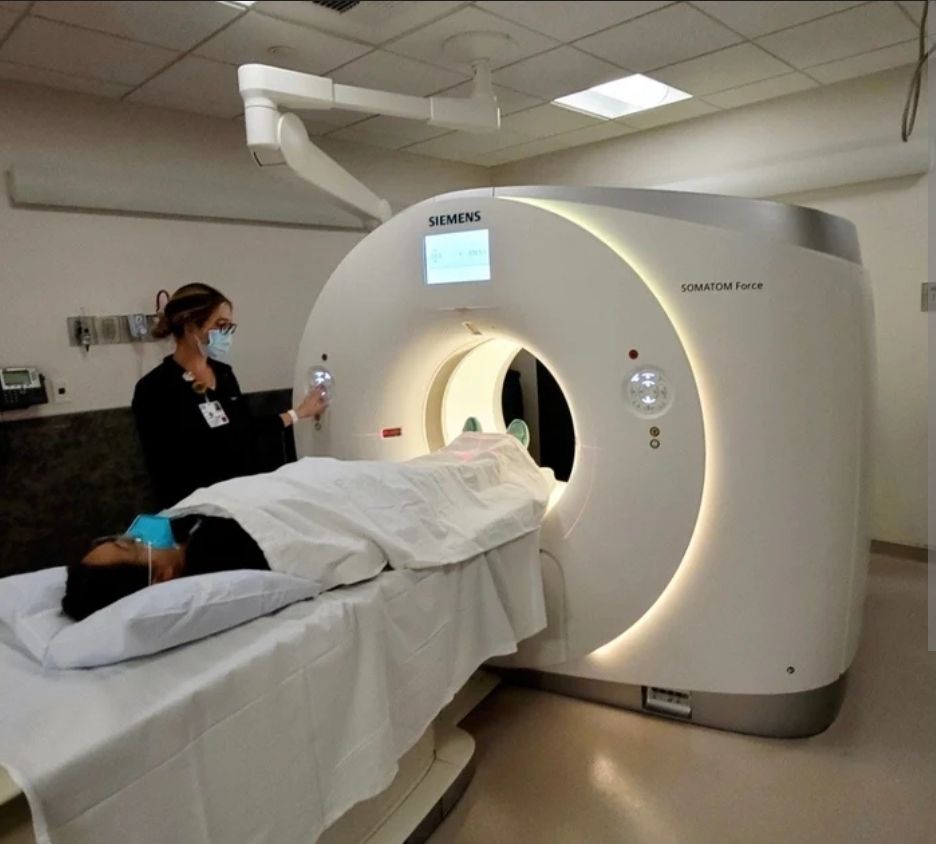
Step 4: Advanced Imaging (When Necessary)
Most ear infections do not need scans.
However, imaging becomes important if:
Infections are recurrent
Complications are suspected
There is persistent discharge
Tumour or cholesteatoma is suspected
CT scans evaluate bone structures. MRI assesses inner ear and nerve involvement.
These investigations are ordered selectively, based on findings.
Step 5: Laboratory Tests (Rare Cases)
Blood tests are rarely needed for simple ear infections.
However, in severe cases or immune-compromised patients, further testing may be appropriate.
Sudden sensorineural hearing loss may sometimes require additional investigations to rule out systemic causes.
Why Proper Diagnosis Matters
Let me explain something important.
Not all ear infections need antibiotics. Not all hearing loss needs hearing aids.
Misdiagnosis leads to:
-Antibiotic resistance
-Chronic inflammation
-Delayed recovery
-Permanent hearing damage
Evidence-based ENT care focuses on identifying the exact problem before prescribing treatment.
Think of it like repairing a car. You don’t replace the engine if the issue is a blocked fuel line.
Precision saves hearing.

Diagnosis in Children: A Special Note
Children often cannot describe symptoms clearly.
Fluid behind the eardrum may persist without pain. Hearing loss may present only as poor attention.
Objective hearing tests and tympanometry are crucial.
Early detection prevents speech delay and academic impact.

Kuala Lumpur Context
Urban noise exposure, frequent viral infections, and environmental allergies increase diagnostic complexity.
Therefore, proper ENT evaluation in Kuala Lumpur is not optional. It is preventive healthcare.

If you are experiencing ear infection symptoms or hearing loss in Kuala Lumpur, a comprehensive ENT examination and hearing test can provide accurate diagnosis and targeted treatment before permanent damage occurs.
Reviewed by Dr Ameen, ENT Specialist, Kuala Lumpur
References
This article is written based on current evidence and clinical practice standards from leading ENT journals, including The Laryngoscope, JAMA Otolaryngology–Head & Neck Surgery, Otolaryngology–Head and Neck Surgery, Otology & Neurotology, Head & Neck, Clinical Otolaryngology, and European Archives of Oto-Rhino-Laryngology.





























Leave a comment